AI Is Building the Prevention Layer Healthcare Never Had
AI-driven longevity platforms are shifting healthcare from diagnosing disease to continuously measuring and preserving human health over time.

Modern healthcare is extraordinarily good at measuring disease.
But it was never designed to measure health.
Cholesterol. Blood pressure. HbA1c. Liver enzymes. Creatinine. Thyroid-stimulating hormone (TSH). These biomarkers help physicians determine how sick we are — or how close we are to becoming sick. They are essential tools for diagnosing conditions and guiding treatment decisions once disease is present.
But they tell us remarkably little about how healthy we actually are.
This gap is becoming increasingly visible as a new longevity ecosystem begins to emerge. Across diagnostics companies, wearable devices, and preventive health platforms, a growing number of AI-native startups are attempting to answer a different question:
What if we could measure health — not just disease?
A new generation of AI-native health companies is beginning to do exactly that.
Companies like Function Health, Superpower, Mito Health, Lifeforce, TruDiagnostic, and GutID are building platforms that combine expanded biomarker testing, longitudinal health data, and machine learning models to create a more continuous understanding of human biology.
Rather than waiting for disease to appear, these platforms aim to detect early signals of physiological change and help individuals intervene earlier.
In effect, they are beginning to build something healthcare never fully developed: a technology-enabled prevention layer.
Healthcare Was Designed to Treat Disease
To understand why this prevention layer is emerging outside traditional healthcare systems, we need to understand how healthcare infrastructure evolved. Modern healthcare was built around the management of illness. Hospitals, insurance reimbursement models, clinical guidelines, and electronic health record systems were designed to diagnose disease and deliver treatment.
Electronic health record platforms like Epic Systems, Oracle Cerner, and Veradigm serve as the digital backbone of healthcare delivery. But their architecture reflects the system they support: diagnosis codes, treatment plans, prescriptions, procedures, and billing documentation.
These systems are effective at coordinating care once a patient becomes sick. They are far less equipped to monitor the gradual biological changes that occur years — or even decades — before chronic disease develops.
Having worked deploying AI-enabled clinical software into hospital systems, one thing becomes immediately clear: the system is tightly optimized for disease management.
Clinical workflows, regulatory structures, and reimbursement models reinforce this orientation. Prevention, by contrast, has historically been difficult to operationalize within that framework. This structural gap has created space for new models to emerge. AI-native health platforms are beginning to fill the prevention infrastructure that traditional healthcare never built.
The Biomarker Gap
One of the clearest manifestations of this gap lies in the biomarkers healthcare chooses to measure. Traditional medical biomarkers are designed to detect pathology or disease risk. Cholesterol helps assess cardiovascular risk. HbA1c reflects long-term glucose regulation. Liver enzymes signal potential organ stress. Thyroid-stimulating hormone (TSH) helps physicians detect thyroid dysfunction.
These markers answer an important question: Is disease present — or likely to develop? But they rarely capture the broader signals that define how well the body is functioning.
Longevity science is dramatically expanding this biomarker universe. New categories of measurement are emerging, including:
- epigenetic biological age
- continuous glucose variability
- inflammatory biomarker profiles
- microbiome diversity
- metabolic flexibility
- hormone balance
- VO₂ max and cardiorespiratory fitness
- sleep architecture and recovery metrics
Instead of simply detecting disease, these markers attempt to measure physiological resilience and performance. In other words, they begin to quantify health itself.
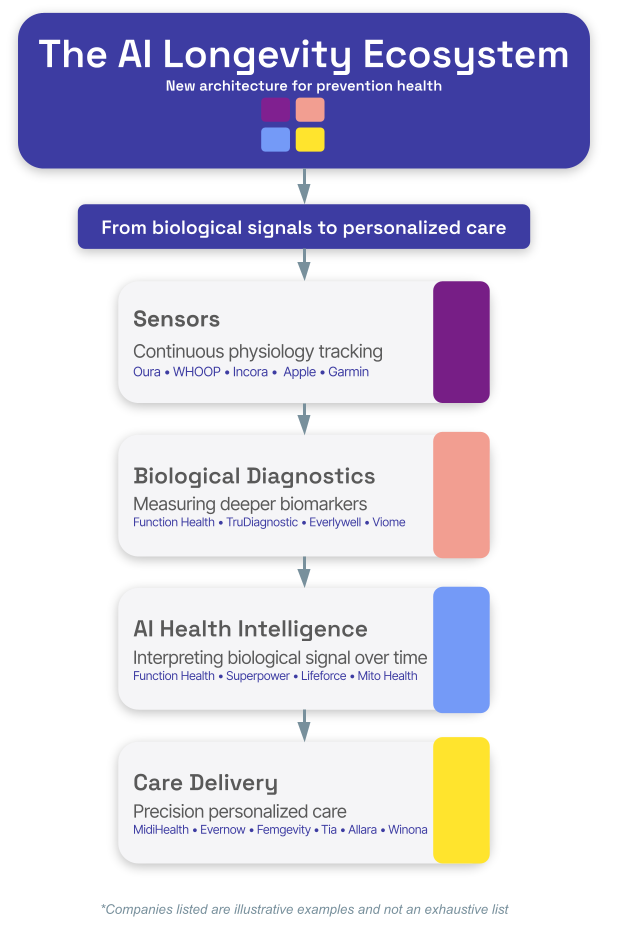
The Evolving AI Longevity Ecosystem
What is emerging is not a single company solving prevention, but an entire technology stack designed to support health optimization.
At the base are biological sensors that collect continuous physiological data. Wearables like the Oura, WHOOP, Incora, and devices from Apple and Garmin track sleep, heart rate variability, recovery, metabolic signals, and menstrual cycles.
Above this layer sit biological diagnostics platforms that measure deeper physiological signals. Companies such as Function Health provide large-scale biomarker panels, while TruDiagnostic measures biological aging through epigenetic testing. Imaging platforms like Ezra are bringing AI-powered full-body scans into preventive health.
The most transformative layer now emerging is AI-powered health intelligence.
AI-native platforms are beginning to aggregate data from wearables, diagnostics, imaging, and lifestyle tracking into unified models of human health. Companies like Superpower and Mito Health are attempting to interpret biological signals across systems, identifying patterns that might otherwise go unnoticed.
Finally, at the top of the stack sits care delivery — clinicians and telemedicine platforms that help patients act on these insights.
Taken together, these layers form what could become the early infrastructure of healthspan
medicine.
Continuous Biological Medicine and Monitoring Instead of Episodic Medicine
Traditional healthcare interactions are episodic. Patients visit doctors during annual checkups or when symptoms appear. Most biological signals remain unmeasured between visits. AI-native health platforms are beginning to shift this model toward continuous biological monitoring.
Wearables track daily physiological patterns. Continuous glucose monitors provide real-time metabolic insights. At-home diagnostics allow individuals to measure hormone levels, inflammation markers, and micronutrients.
AI models can analyze these longitudinal datasets to identify subtle changes over time. Small deviations in metabolic health, inflammatory signals, or sleep patterns may become visible years before they manifest as clinical disease.
Instead of asking “What disease does this patient have?”, these systems begin to ask a different question: “What direction is this person’s biology moving in?”
Women’s Health as a Catalyst for Innovation
One of the fastest-moving areas in this ecosystem is women’s health.
For decades, women navigating hormonal transitions in midlife have faced significant gaps in traditional healthcare systems. Menopause, metabolic changes, and hormone fluctuations were often poorly monitored and under-researched (they still are).
New platforms are stepping in to address this gap. Telemedicine companies like Midi Health, Evernow, Femgevity, and Tia are expanding access to menopause care and hormone expertise. At the same time, data platforms such as Flo and Levels are generating large volumes of longitudinal reproductive and metabolic data.
As these datasets grow, they may become some of the most valuable inputs for AI systems attempting to model human health trajectories — particularly across life stages where traditional medicine has historically lacked insight.
Women’s health may ultimately become one of the most powerful catalysts for the development of the AI longevity stack.
A System at an Inflection Point
The longevity movement is sometimes dismissed as a niche interest of biohackers and wellness enthusiasts. But a closer look suggests something more structural is happening. Our healthcare system is effective at treating disease once it occurs. Yet it has historically invested far less energy in understanding how to maintain optimal human health over decades. AI-native longevity companies are beginning to explore that frontier.
By expanding the biomarkers we measure, collecting continuous biological data, and applying machine learning to human physiology, these platforms are beginning to map the space between being sick and being truly well.
In doing so, they may be building something healthcare never fully developed: a system designed not only to treat disease, but to maintain health. If this prevention layer continues to mature, the central question of medicine may begin to shift. Not simply how we treat illness — but how we preserve optimal human function for as long as possible.
Ashley Schmidt, MSPH works at the intersection of AI, healthcare systems, and technology innovation. She has led enterprise deployments of AI-driven clinical software across major U.S. health systems, including the Cleveland Clinic, and supported global AI platforms focused on health system forecasting and supply chain optimization. She was a founding member of a health marketplace focused on women’s health and longevity, starting with perimenopause and menopause. Her career began at the World Health Organization and spans more than 15 years, advancing innovative health solutions for underserved populations.
